Resident Didactics
Grand Rounds occurs every Wednesday morning from 6:30 AM – 7:30 AM. We often have visiting professor lectures on Tuesday nights for residents if the Grand Rounds presenter has a topic area they would like to present on.
We have protected education time occurring every Monday afternoon starting at 4:30 PM. During this time,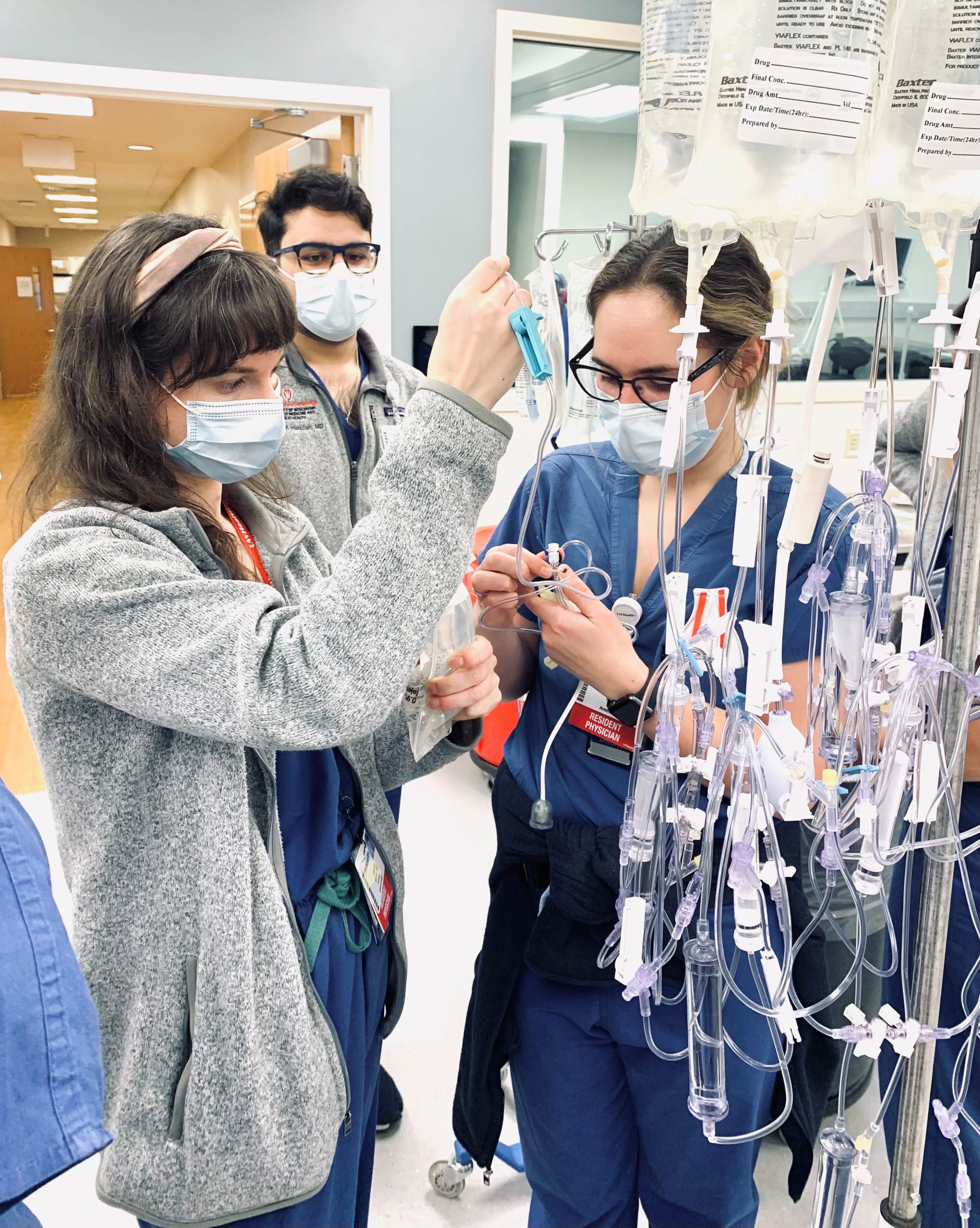 we have monthly Morbidity and Mortality conferences, monthly Journal Clubs, weekly Case Conference series, and monthly Simulation Sessions. We model most of our education sessions after our highly rated Case Conference series, where we alternate between anesthesia subspecialties presenting interesting cases that have occurred at our institution and supporting literature on the management of them. In 2019, we introduced our new monthly simulation curriculum that consists of a pre-simulation lecture, multiple simulation sessions based on PGY year, and a post-simulation lecture.
we have monthly Morbidity and Mortality conferences, monthly Journal Clubs, weekly Case Conference series, and monthly Simulation Sessions. We model most of our education sessions after our highly rated Case Conference series, where we alternate between anesthesia subspecialties presenting interesting cases that have occurred at our institution and supporting literature on the management of them. In 2019, we introduced our new monthly simulation curriculum that consists of a pre-simulation lecture, multiple simulation sessions based on PGY year, and a post-simulation lecture.
In addition to the Monday protected education time, we have CA 1 Basic exam and CA2/3 Advanced exam didactic sessions that are a mixture of in-person lectures and podcasts from multiple sources.
The Department of Anesthesiology has a robust Oral Boards curriculum, with many faculty serving as ABA board examiners. We perform formal Mock Oral exams about 4 to 5 times per year.
Resident Simulation Education
Simulation education provides a safe learning environment to develop and enhance procedural knowledge and efficiency, teach crisis management, and provide training to deal with difficult patient, patient family, and colleague situations. Throughout their training, University of Wisconsin residents participate in a multitude of simulation activities. During PGY-1 year, interns engage in simulations run by anesthesiology faculty to practice procedural skills, such as central line placement and advanced airway management, as part of their ongoing 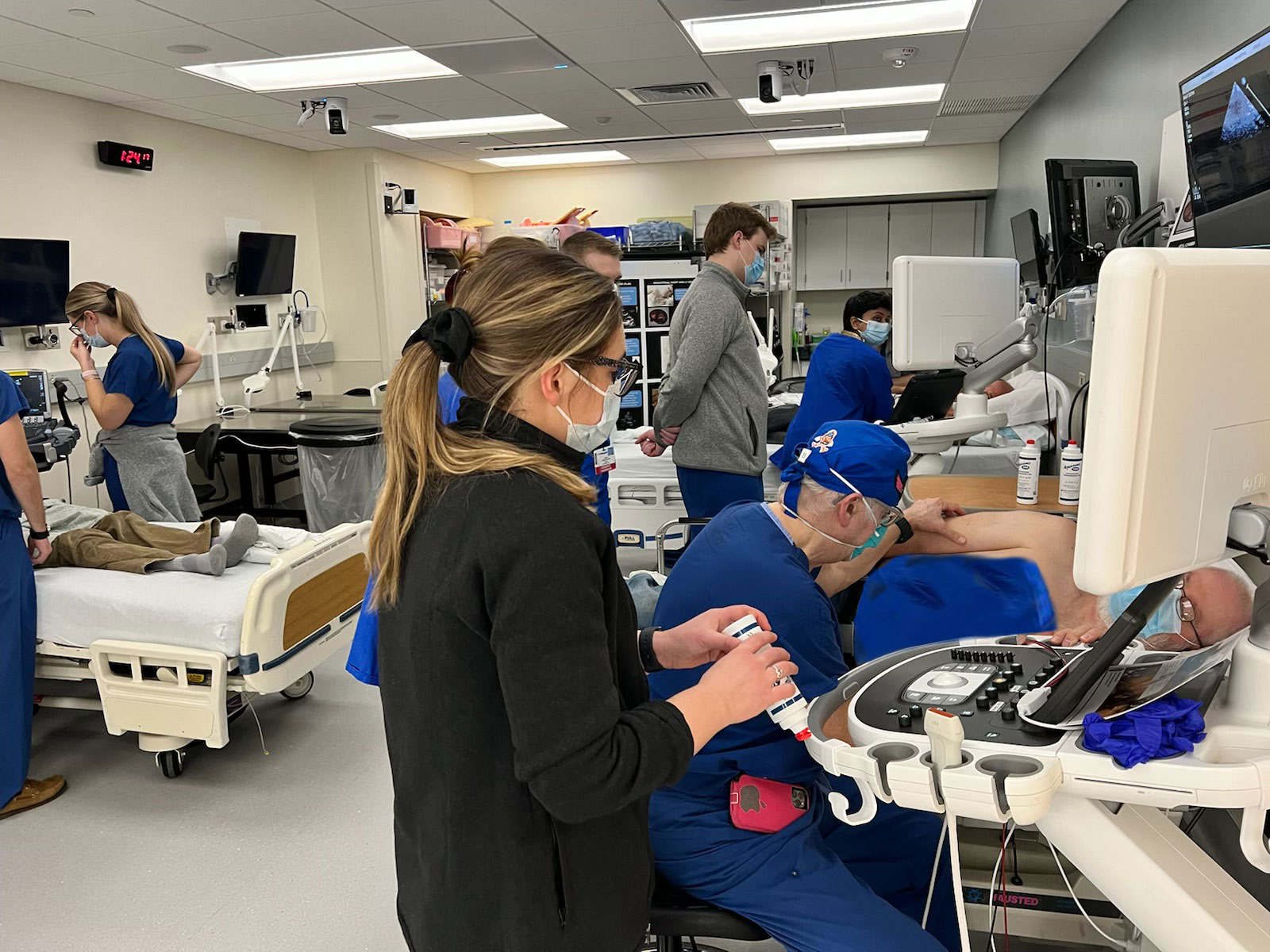 integrated anesthesiology education. During the clinical anesthesia years, residents participate in simulation sessions every other month to actively train for crisis scenarios and rare anesthesia-related events, such as malignant hyperthermia, anaphylaxis, pulmonary embolus, massive surgical hemorrhage, airway fire, intra-operative ischemia, local anesthetic systemic toxicity, difficult intubation/cannot intubate-cannot ventilate, and out-of-operating room airway management. Residents also get practice in difficult patient scenarios, including relaying difficult news, obtaining informed consent, and discussing perioperative Do Not Resuscitate situations. In addition to the formal simulation curriculum, a HeartWorks simulator supplements residents’ hands-on training with transthoracic and transesophageal echocardiography. Also, in preparation for the ABA APPLIED examination, residents participate in full-length exemplary anesthesia objective structured clinical examinations (OSCEs) to ensure excellent preparation for this third exam in the Staged Exam series for board certification.
integrated anesthesiology education. During the clinical anesthesia years, residents participate in simulation sessions every other month to actively train for crisis scenarios and rare anesthesia-related events, such as malignant hyperthermia, anaphylaxis, pulmonary embolus, massive surgical hemorrhage, airway fire, intra-operative ischemia, local anesthetic systemic toxicity, difficult intubation/cannot intubate-cannot ventilate, and out-of-operating room airway management. Residents also get practice in difficult patient scenarios, including relaying difficult news, obtaining informed consent, and discussing perioperative Do Not Resuscitate situations. In addition to the formal simulation curriculum, a HeartWorks simulator supplements residents’ hands-on training with transthoracic and transesophageal echocardiography. Also, in preparation for the ABA APPLIED examination, residents participate in full-length exemplary anesthesia objective structured clinical examinations (OSCEs) to ensure excellent preparation for this third exam in the Staged Exam series for board certification.