Research in my lab centers on how pain is pervasive and devastating. Poorly treated chronic pain is the largest source of disability in America with an estimated economic cost in excess of 500 billion dollars per year. Moreover, existing strategies to disrupt pain (e.g. opiates) have well known and highly undesirable effects on reward circuits in the CNS. Better strategies for preventing chronic pain are desperately needed.
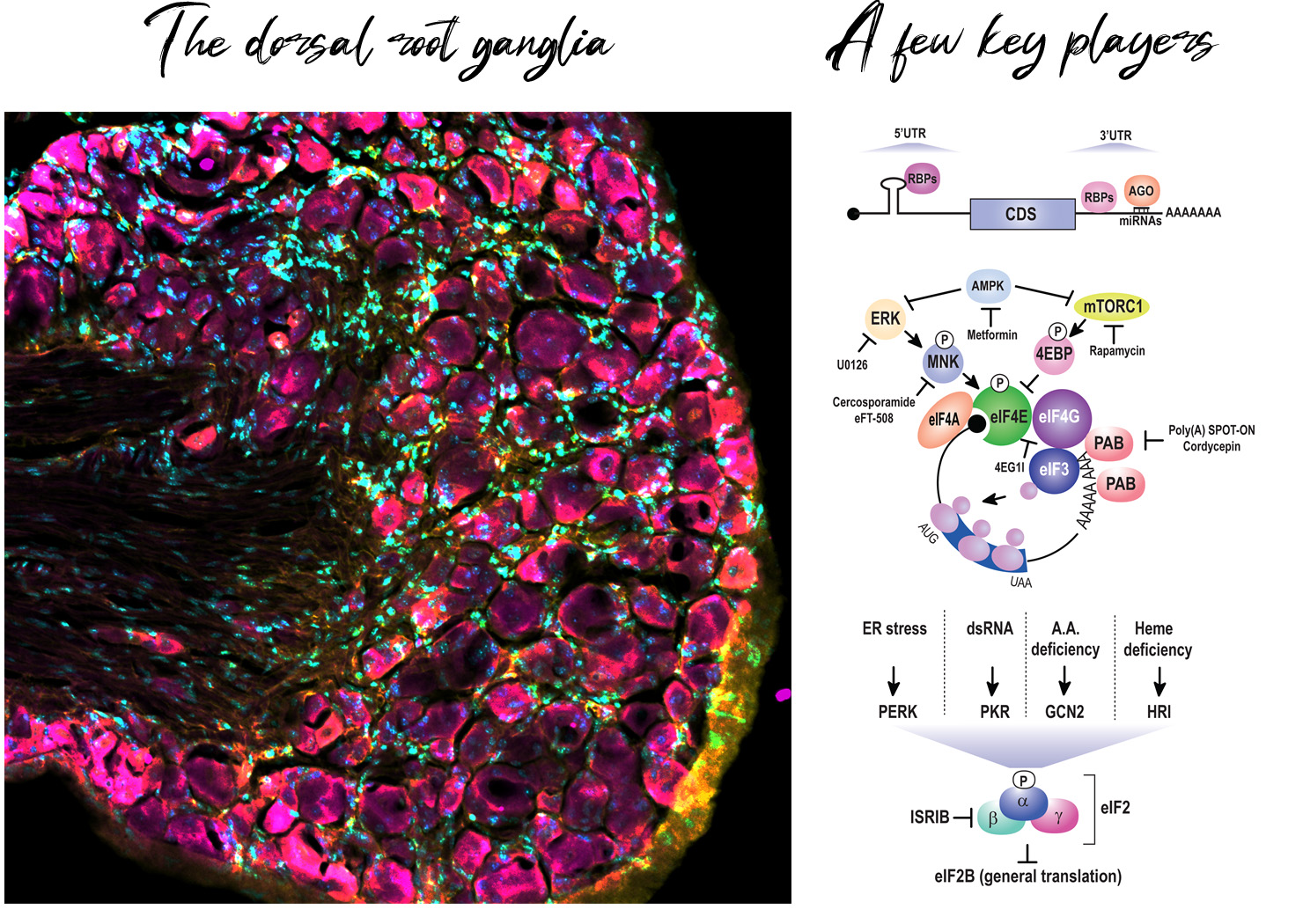
In the vast majority of cases, pain originates in the periphery in a specialized type of sensory neuron called a nociceptor. Long-lived changes in their excitability – which are intimately liked to chronic pain – require de novo protein synthesis. Multiple groups have shown that peripheral inhibition of protein synthesis diminishes pain associated behaviors in pre-clinical rodent models. This suggests that translation, likely in nerve fibers, is critical for nociceptive plasticity. But what are the mRNAs that need to be locally translated and what governs the specificity of protein synthesis in nociceptors?
To address these key questions, we make use of functional genomics, pharmacology, physiology, and genetic approaches.
More Info

Zachary Campbell, PhD
Associate Professor
Department of Anesthesiology
University of Wisconsin
(608) 263-8100